- Family Care Coordinators (FCC)-All families and youth enrolled with the CME must choose an FCC to work with during their enrollment with the CME
- Family Support Partner (FSP)
- Youth Support Partner (YSP)
- Respite Providers
Children already eligible for Wyoming Medicaid may apply for CME services directly with Magellan. For more CME information, please visit https://www.magellanofwyoming.com or contact Magellan via e-mail at: WyomingInfo@MagellanHealth.com or call the customer service center at: 1-855-883-8740 [TDD/TTY: 1-800-424-6259]. Children not currently financially eligible for Wyoming Medicaid and who meet clinical eligibility criteria for CME services may also apply for participation in through the CMHW program by enrolling in the Children’s Mental Health Waiver. The financial qualification is determined based solely on the child/youth’s own income and resources.
Qualifications for Children and /Youth to be Served by the Care Management Entity
- Children and youth between the ages of 4-21
- Meets the definition of serious emotional disturbance or serious mental illness
- Meets at least one Medicaid criteria for inpatient psychiatric hospitalization
- CASII composite score of 20-27 (between ages of 6-20) or a score of 18 or > on the ECSII (ages 4-5)
Helpful Links
By using this website, you acknowledge that the State of Wyoming does not endorse any of the sites or services that may be referenced on or linked to on this site. The State of Wyoming will not be responsible or liable for those sites’ content or any loss occasioned by any such content. Other Internet sites or services may have privacy policies or security that differ from the privacy policy or security of the State of Wyoming.
CME Reports, Audits and Notices
External Quality Review Audits
SFY25. Federal regulation mandates states to conduct an annual external quality review (EQR) of Medicaid services delivered through managed care entities. Wyoming Medicaid contracted with Guidehouse Inc. as the external quality review organization (EQRO) to perform the external quality review of Magellan Healthcare Inc. for services delivered in State Fiscal Year (SFY) 2025 and produce this Technical Report and appendices as set forth in 42 CFR § 438.364.
SFY24. Federal regulation mandates states to conduct an annual external quality review (EQR) of Medicaid services delivered through managed care entities. Wyoming Medicaid contracted with Guidehouse Inc. as the external quality review organization (EQRO) to perform the external quality review of Magellan Healthcare Inc. for services delivered in State Fiscal Year (SFY) 2023 and produce this Technical Report and appendices as set forth in 42 CFR § 438.364.
SFY23. Federal regulation mandates states to conduct an annual external quality review (EQR) of Medicaid services delivered through managed care entities. Wyoming Medicaid contracted with Guidehouse Inc. as the external quality review organization (EQRO) to perform the external quality review of Magellan Healthcare Inc. for services delivered in State Fiscal Year (SFY) 2023 and produce this Technical Report and appendices as set forth in 42 CFR § 438.364.
SFY22. Federal regulation mandates states to conduct an annual external quality review (EQR) of Medicaid services delivered through managed care entities. Wyoming Medicaid contracted with Guidehouse Inc. as the external quality review organization (EQRO) to perform the external quality review of Magellan Healthcare Inc. for services delivered in State Fiscal Year (SFY) 2022 and produce this Technical Report and appendices as set forth in 42 CFR § 438.364.
SFY21. Federal regulation mandates states to conduct an annual external quality review (EQR) of Medicaid services delivered through managed care entities. Wyoming Medicaid contracted with Guidehouse Inc. as the external quality review organization (EQRO) to perform the external quality review of Magellan Healthcare Inc. for services delivered in State Fiscal Year (SFY) 2021 and produce this Technical Report and appendices as set forth in 42 CFR § 438.364.
SFY20. Description: Federal regulation mandates states to conduct an annual external quality review (EQR) of Medicaid services delivered through managed care entities. Wyoming Medicaid contracted with Guidehouse Inc. as the external quality review organization (EQRO) to perform the external quality review of Magellan Healthcare Inc. for services delivered in State Fiscal Year (SFY) 2020 and produce this Technical Report and appendices as set forth in 42 CFR § 438.364.
SFY19. Federal regulation mandates states to conduct an annual external quality review (EQR) of Medicaid services delivered through managed care entities. Wyoming Medicaid contracted with Guidehouse Inc. as the external quality review organization (EQRO) to perform the external quality review of Magellan Healthcare Inc. for services delivered in State Fiscal Year (SFY) 2019 and produce this Technical Report as set forth in 42 CFR § 438.364.
Annual Accreditation
The federal government requires each state Medicaid agency to publicly post whether any managed care entity contract with the state has been accredited by a private independent accrediting entity and post that information annually on their website. This posting verifies that the state’s Care Management Entity has not been accredited by a private independent accrediting entity specific to the work performed under the contract with the state Medicaid agency.
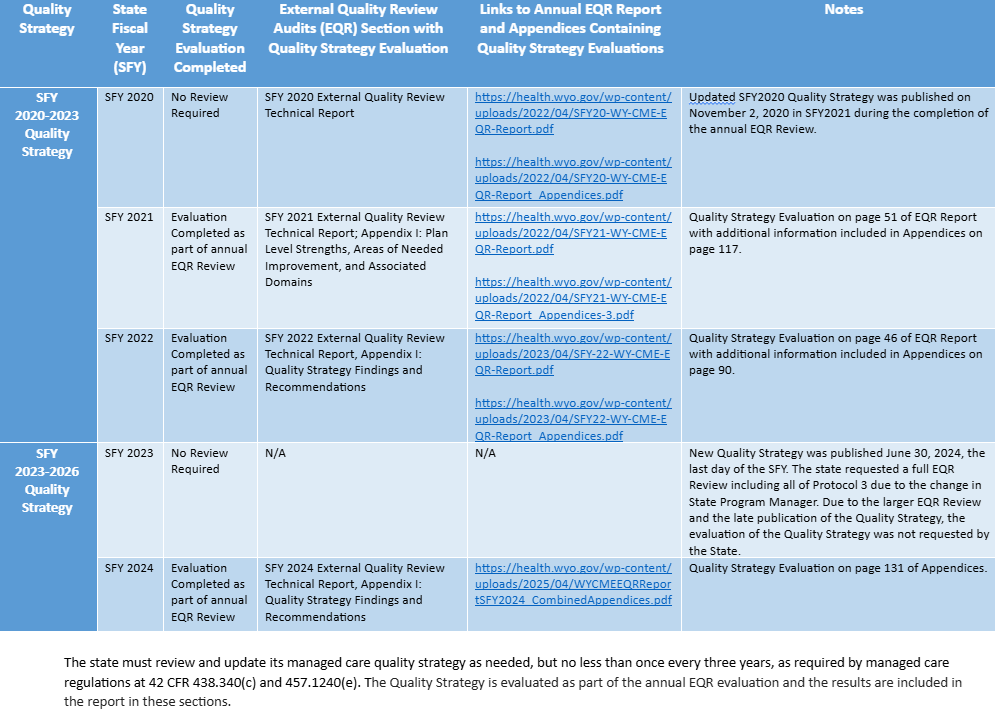
Quality Review Strategy Table
To access the linked Annual EQR Report & Appendices Containing Quality Strategy Evaluations in the table below, please CLICK HERE.
Page last updated on April 29, 2026.

