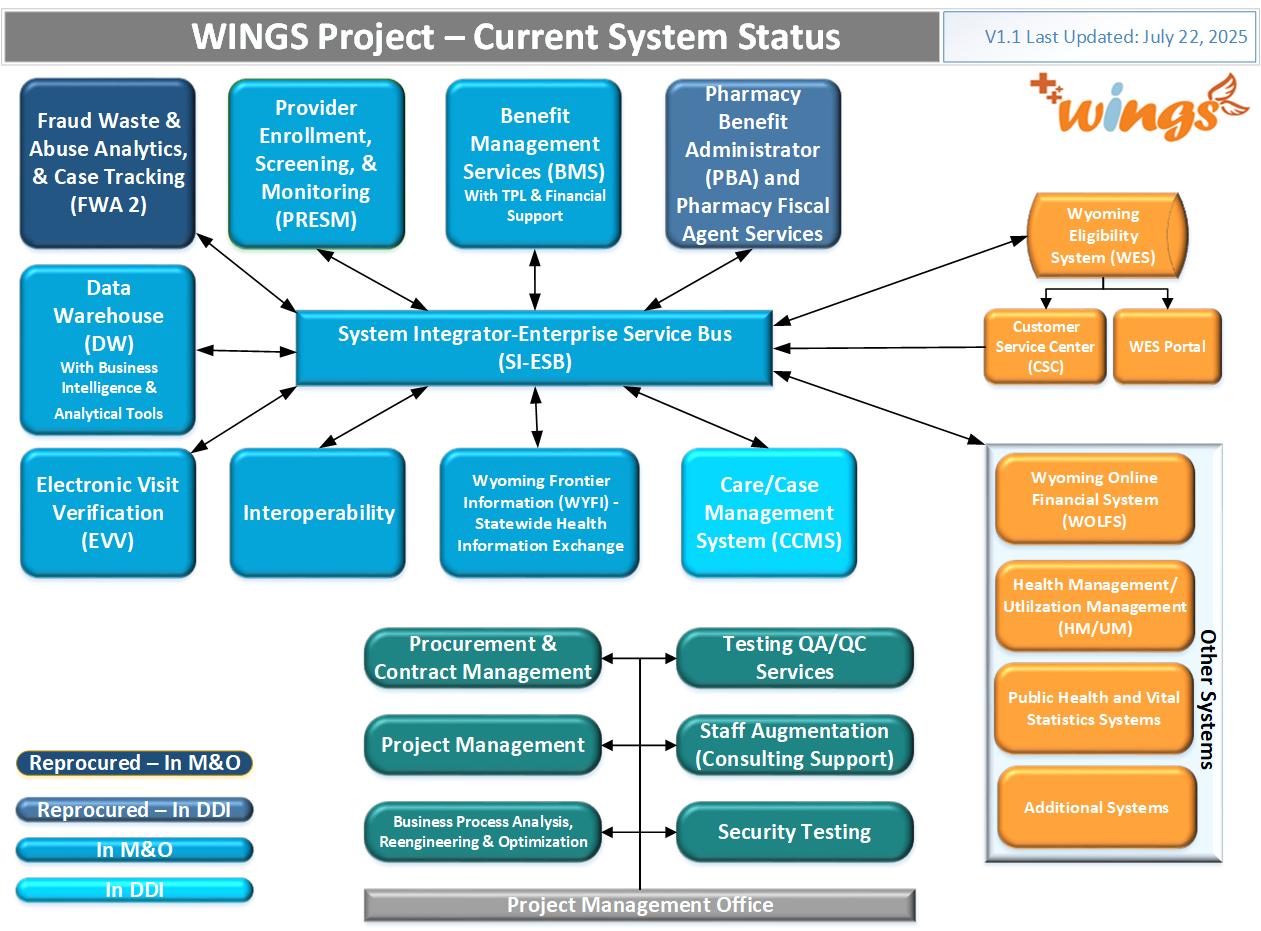
The Wyoming Integrated Next Generation System (WINGS) will replace the current Medicaid Management Information System (MMIS) through separate procurements, represented in the “WINGS Project—To-Be Vision” graphic (above). The WINGS project modules will be procured over the next two to three years. See below for current information on each procurement.
Pharmacy Benefit Management System (PBMS)
Overview: PBMS processes pharmacy point-of-sale claims and handles pharmacy related prior authorizations, among other duties. The new PBMS system replaced the previous PBMS system and services with the latest system functionality, features, and new services to better meet the needs of the State as well as those of Wyoming Medicaid’s pharmacy providers and clients. The PBMS replacement has helped the State achieve greater efficiencies and cost-effective utilization, improve patient health outcomes and to increase fraud, waste and abuse detection capabilities.
Module Status: The system went live on July 23, 2017, and has continued to operate successfully and efficiently with no unplanned downtime since go-live. The State formally accepted the PBMS system on October 24, 2017, and CMS approved system certification on February 1, 2019.
Contract Holder: Change Healthcare (CHC), formerly Goold Health Systems (GHS)
This page was last updated: 03/26/2024
System Integrator with Enterprise Service Bus (SIESB)
Overview: The SI/ESB component connects all of the modules together into an enterprise system so that the WINGS vision can be realized. It encompasses three main areas: Systems Integration and Enterprise Service Bus, Technical Coordination, and Data Management Services. The SI/ESB Contractor is instrumental in the transition from the current MMIS environment to the desired WINGS vision including the essential communication, cooperation, and collaboration with other WINGS project Contractors and the State for successful integration outcomes.
Module Status: The SI/ESB contract was executed on October 10, 2017, and project kick-off activities began in November 2017. The initial technical platform was stood up in the fall of 2018, and the system is now in production. The SI/ESB entered O&M on May 1, 2019, and is fully integrated with the Data Warehouse. Currently the system is live and is going system integrations.
Contract Holder: Deloitte Consulting LLP
This page was last updated: 03/26/2024
Data Warehouse with Business Intelligence Tools (DW/BI)
Overview: The Data Warehouse serves as the main data storage repository for all the other WINGS Project modules (with the intention of bringing in data from other Department of Health areas over time). Business Intelligence Tools will be utilized to access this stored data to compile reports and analyze Medicaid program information to help inform Agency decision making. This module will replace and enhance the current data warehouse solution, including new and/or expanded data analytics, business intelligence tools, and reporting capabilities.
Module Status: The DW/BI contract was executed on March 8, 2018, and project kick off activities began that month. The initial data warehouse technical framework/platform was set up in late 2018, and integration with the System Integrator occurred in early spring 2019. The Data Warehouse entered O&M on March 1, 2019. Currently the system is live and is going in system integration.
Contract Holder: Deloitte Consulting LLP
This page was last updated: 03/26/2024
Independent Verification and Validation (IV&V)
Overview: The IV&V vendor helps the State to meet project responsibility requirements, objectives, milestones, and deliverables for all procured WINGS project components and phases to ensure systems, products, or services meet the State’s intended purpose, requirements and user needs and can ultimately obtain CMS certification. In accordance with CMS guidance, the IV&V services must be provided and managed by an organization that is technically and managerially independent of the State and WINGS project vendors.
Module Status: The IV&V contract was executed on February 10, 2017, with SLI Global Solutions, and project kick-off activities began in March 2017. To date, SLI has delivered their required project documents, and reviewed and assessed component module documentation for the PBMS, SI/ESB, DW/BI-R, FWA, and PRESM modules. IV&V continues to participate in start-up, milestone, and general reviews, and work with the State to improve processes and provide cyclical updates to CMS.
Contract Holder: SLI Global Solutions
This page was last updated: 12/24/2019
Fraud, Waste, Abuse Analytics and Case Tracking (FWA)
Overview: The FWA system replaces and enhances the previously existing FWA tool and applications to improve overall detection and recovery functions as well as administrative activities and financial reporting.
Module Status:
Contract Holder: Alivia Analytics LLC
This page was last updated: 07/22/2025
Provider Enrollment, Screening, and Monitoring (PRESM)
Overview: The PRESM module provides a solution to streamline the internal and external user’s experience through consolidation, enhancement, and automation of existing provider enrollment processes. Providers conduct enrollment and revalidation business through a self-service, web-based portal. Through the portal, providers will be able to complete a single online application and track submitted enrollment. The online portal also allows providers to manage their provider record data through Change of Circustance (CoC) requests.
Module Status: This module was originally intended to fall within the scope of the BMS procurement, but market research and vendor input led the Agency to conclude that the best option was to procure a COTS product to perform this function. The State participated in a Provider Services multi-state cooperative procurement with Montana and several other states in order to procure the PRESM module off a NASPO ValuePoint purchasing list. The PRESM contract was executed on August 23, 2019, with HHS Technology Group, LLC. The PRESM solution went live to the public as of April 21, 2021.
Contract Holder: HHS Technology Group, LLC
This page was last updated: 03/26/2024
Benefit Management Service (BMS)
Overview: The BMS vendor will conduct and manage claims processing and supporting services. The vendor will perform related administrative functions to the overall operational and business process, as well as online provider enrollment, provider call center and help desk, including Interactive Voice Response (IVR) software, and case management services. The vendor will use system reporting for program oversight, budgeting, and review. The BMS Vendor will also incorporate an all-inclusive Third Party Liability (TPL) services-specific Contractor solution to receive TPL claims and information from internal/external sources and match data and maintain members’ TPL and support recovery processes.
Module Status: The BMS contract executed March 20, 2020, with Client Network Services, and project kick-off activities began in March 2020. Currently the system is live since October 2021.
Contract Holder: Client Network Services (CNSI)
This page was last updated: 03/26/2024
Electronic Visit and Verification (EVV)
Overview: This system provides a verification mechanism to the State for service types established under the 21st Century Cures Act for type of service performed; individual receiving the service; date of the service; location of service delivery; individual providing the service; and time the service begins and ends. Outreach and education to system users took place across the State in advance of project implementation. The State applied a two-pronged approach to meeting the need for EVV that entailed enhancements to an existing system for self-directed providers, as well as the procurement of a statewide vendor for EVV service providers.
Module Status: The EVV contract was executed September 1, 2020 with Carebridge. The system went live as of February 15, 2022.
Contract Holder: CareBridge Health
This page was last updated: 03/26/2024
Hello WINGS Project Vendors and Potential Vendors,
We want to keep you informed! If you are interested in receiving vendor fair notifications and periodic WINGS newsletters, please let us know you’d like to be put on our vendor list by signing up here:
Link to WINGS Vendor Sign-Up Form.
If you are already on the WINGS Vendor List, but have not registered for Public Purchase (application used to view Agency open RFPs and submit a RFP vendor proposal). Sign up here:
We anxiously await your proposals once a RFP has been released. Please follow the instructions provided within the RFP and Public Purchase when submitting your proposal(s). As a friendly reminder, if you do not follow the instructions for submitting your proposal(s), or if you send your proposal directly to any Wyoming Department of Health staff, including the Wyoming Department of Health Director, your proposal will not be considered.
We look forward to your submissions.
Sincerely,
The WINGS Team
The WINGS project is focused on you, potential and existing Medicaid clients. Our WINGS project team will not rest until our goal of streamlining and enhancing the current Medicaid service delivery system is replaced with a more integral approach to processing claims; discovering instances of fraud, waste, and abuse of Medicaid services; assisting Medicaid clients with third party liability; and other components. Over the life of the WINGS project, we will fold in other Department of Health areas in order to move away from a “siloed” healthcare approach and integrate into a comprehensive view of understanding the health of not only Medicaid clients, but all Wyoming’s citizens.
We know that spending taxpayer money (it’s our money too) is delicate, especially in these tough economic times. We are extremely conscientious of this fact, and consider it an honor to wisely use a bit of Wyoming’s general fund money. Please know that we have taken full advantage of enhanced federal funding. As you may have read in the Advanced Planning Document (APD) within the Document Library on this webpage, this enhanced federal funding will fluctuate during different project phases. You’ll see that WINGS will receive (federal funds/general funds percentages) 90/10, 75/25, and 50/50 funding. We are ensuring Wyoming’s money stretches as far as it can.
What does this mean for you? As the WINGS project gains momentum, we hope you don’t notice much. What we mean is, yes, this project will touch thousands of people, but we don’t anticipate interruptions to “business as usual.” Our vision is a seamless one, with gradual ascension.
We are in service to you.
Sincerely,
Your WINGS Team
Status Update for Project Activities This status update report provides general information about anticipated WINGS project activities and time lines for various procurements. The status report will be posted periodically with updated information and time frames for key focus areas that may be of interest to Medicaid vendors.
WINGS Project Glossary of Terms and Abbreviations This document is for information only and contains acronyms, terms, and definitions that are commonly used in Wyoming Medicaid and WINGS Project procurements.
Procurement Strategy Executive Report This report contains Wyoming MITA 3.0 State Self-Assessment information and outcomes as well as Medicaid Management Information System (MMIS) alternative strategies based on research and vendor feedback from the Medicaid Claims Processing and Related Medicaid Administrative Services questionnaire responses received in January 2015. Wyoming Medicaid WINGS project procurement strategy for the next three years, is also included in this summary report.
Data Warehouse Takeaways This document contains descriptions of items covered and functionality demonstrated during the October 2014 Data Warehouse/Business Intelligence vendor fair.
Pharmacy Vendor Fair Takeaways This document contains descriptions of items covered and functionality demonstrated during the October 2014 pharmacy vendor fair.
Fraud, Waste and Abuse Takeaways This document contains descriptions of items covered and functionality demonstrated during the June and August 2015 Fraud, Waste, Abuse vendor fair.
Advanced Planning Document This document contains the first Implementation Advance Planning Document (IAPD) request to Centers for Medicare and Medicaid Services (CMS) for funding approval for WINGS project activities. CMS approved IAPD v3.1 on September 12, 2019. This IAPD provided updates for all WINGS modules and folded in the Electronic Visit Verification (EVV) project. This IAPD will be updated on an ongoing basis to reflect pertinent changes to WINGS project scope, schedule, and budget.
For those who are interested in Wyoming Department of Health procurement activities and timelines, please note they are subject to change–please see Public Purchase for official Request for Proposal (RFP) notices and releases, and stay tuned for future updates!
The documents contained herein are visionary in nature, and can be changed at the sole discretion of the State. This page was last updated on July 22, 2025.